SERVICES
- Allergy Screening
- Chemical Peels
- Dermapen
- Facial Skin Analysis
- FreshEyes
- Hyperhidrosis (Excessive Sweating)
- Hair Loss Treatment
- Laser Clinic
- Liquid Facelift
- Keloid Treatments
- Medical Facials
- Medical Treatments
- Mole Mapping
- Photodynamic Therapy (PDT)
- Skincare Advice
- Pigmentation Treatment
- Surgical Procedures
- Ultraviolet Phototherapy
USEFUL LINKS
What is a basal cell carcinoma?
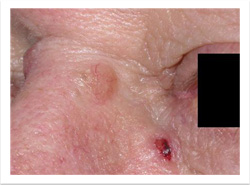 A basal cell carcinoma is a type of skin cancer – the most common one in South Africa. It is sometimes also called a ‘rodent ulcer’.
A basal cell carcinoma is a type of skin cancer – the most common one in South Africa. It is sometimes also called a ‘rodent ulcer’.
What causes basal cell carcinoma?
The commonest cause is too much exposure to ultraviolet (UV) light from the sun or from sun beds. Basal cell carcinomas can occur anywhere on your body, but are most common on areas that are exposed to the sun, such as your face, head, neck and ears. It is also possible for a basal cell carcinoma to develop where burns, scars or ulcers have damaged the skin. Basal cell carcinomas are not infectious.
Basal cell carcinomas mainly affect fair skinned adults and are more common in men than women. Those with the highest risk of developing a basal cell carcinoma are:
- People with freckles or with pale skin and blond or red hair.
- People who use sun beds.
- Those who have had a lot of exposure to the sun, such as people with outdoor hobbies or who work out of doors, and people who have lived in sunny climates
People who have previously had a basal cell carcinoma.
Are basal cell carcinomas hereditary?
Apart from a rare familial condition called Gorlin’s syndrome, basal cell carcinomas are not hereditary. However some of the things that increase the risk of getting one (e.g. a fair skin, a tendency to burn rather than tan, and freckling) do run in families.
What are the symptoms of basal cell carcinomas?
Most basal cell carcinomas are painless. People often first become aware of them as a scab that bleeds occasionally and does not heal completely. Some basal cell carcinomas are very superficial and look like a scaly red flat mark: others have a pearl-like rim surrounding a central crater. If left for years, the latter type can eventually erode the skin causing an ulcer — hence the name “rodent ulcer”. Other basal cell carcinomas are quite lumpy, with one or more shiny nodules crossed by small but easily seen blood vessels.
How will my basal cell carcinoma be diagnosed?
Sometimes the diagnosis is clear from its appearance. If further investigation is necessary a small area of the abnormal skin (a biopsy) or all of the lesion (an excision biopsy) may be cut out and examined under the microscope. You will be given a local anaesthetic beforehand to numb the skin.
Can basal cell carcinomas be cured?
Yes, basal cell carcinomas can be cured in almost every case, although treatment becomes complicated if they have been neglected for a very long time, or if they are in an awkward place – such as near the eye, nose or ear. Seldom, if ever, do they spread to other parts of the body.
How can a basal cell carcinoma be treated?
The commonest treatment for basal cell carcinoma (BCC) is surgery. Usually, this means cutting away the BCC, along with some clear skin around it, using local anaesthetic to numb the skin. Sometimes, a small skin graft is needed.
Another type of surgery is Mohs micrographic surgery. This involves the excision of the affected skin that is then examined under the microscope straight away to see if all the BCC has been removed. If any residual BCC is left at the edge of the excision further skin is excised from that area and examined under the microscope and this process is continued until all the BCC is removed. The site is then usually covered with a skin graft. This is a time consuming process and only undertaken for certain BCCs in difficult anatomical areas if simple surgery is not suitable. ]
Other types of treatment include:
- Curettage and cautery — the skin is numbed with local anaesthetic and the BCC is scraped away (curettage) and then the skin surface is sealed (cautery).
- Cryotherapy – freezing the BCC with a very cold substance (liquid nitrogen).
- Radiotherapy — shining X-rays onto the area containing the BCC.
- Creams — these can be applied to the skin. The two most commonly used are 5-fluorouracil (5-FU) and imiquimod.
- Photodynamic therapy — A special cream is applied to the BCC which is taken up by the cells that are then destroyed by exposure to a specific wavelength of light.
- This treatment is only available in certain dermatology departments.
Surgical excision is the preferred treatment but the choice of treatment depends on the site and size of the BCC, the condition of the surrounding skin and number of BCCs to be treated (some people have many) as well as the overall state of health of each person to be treated.
What can I do?
Treatment will be much easier if your basal cell carcinoma is detected early. It is advisable to see your doctor if you have any marks or scabs on your skin which are:
Growing, bleeding, never completely healing or changing appearance in any way. Check your skin for changes once a month. A friend or family member can help you particularly with checking your back.
You can also take some simple precautions to help prevent a basal cell carcinoma appearing:
Top sun safety tips
- Protect the skin with clothing, including a hat, T shirt and UV protective sunglasses
- Spend time in the shade between 11am and 3pm when it’s sunny
- Use a ‘high protection’ sunscreen of at least SPF 30 which also has high UVA protection, and make sure you apply it generously and frequently when in the sun.
- Keep babies and young children out of direct sunlight
- The British Association of Dermatologists recommends that you tell your doctor about any changes to a mole — if your GP is concerned about your skin, make sure you see a Consultant Dermatologist (on the GMC register of specialists), the most expert person to diagnose a skin cancer. Your GP can refer you via the NHS.
Sunscreens should not be used as an alternative to clothing and shade, rather they offer additional protection. No sunscreen will provide 100% protection.
Patient Testimonials
EXCELLENTTrustindex verifies that the original source of the review is Google. From my first visit with Dr Jhetam I knew I would go back. He is compassionate , friendly and has an interaction which made you feel comfortable. This is very important in any doctor because our relationship with our doctor is very intimate.Trustindex verifies that the original source of the review is Google. Dr Jhetman is truly one of a kind. Anyone who is fortunate enough to be in his care can so grateful. Academic, informative and reassuring. It’s hard to find a doctor who has this combination of skills these days. He dealt with my Melonoma concerns with swift and professional care. And his staff are equally as competent and caring. I cannot commend Dr Jhetman and his staff enough on true patient care. Thank you!Trustindex verifies that the original source of the review is Google. I was absolutely satisfied with my experience with Dr Jhetham & his winning team. Keep up the good work.Trustindex verifies that the original source of the review is Google. Best skin doctor..Dr Jetham prescribed the best products that have brought so much of a glow to my skin..being a transplant patient and so much happening to my skin just 4 visits to him and my face is back to it's radiance ..I hightly reccomend Dr Jetham ...you won't go wrong..Trustindex verifies that the original source of the review is Google. Dr. Imraan Jhetam and his team provided exceptional care, showcasing professionalism and compassion in every interaction. Dr. Jhetam took the time to thoroughly explain everything, addressing each of my concerns with empathy and understanding. My experience with him was truly wonderful, and I highly appreciate his dedication to patient care.Verified by TrustindexTrustindex verified badge is the Universal Symbol of Trust. Only the greatest companies can get the verified badge who has a review score above 4.5, based on customer reviews over the past 12 months. Read more