What is a fungal infection of the nail?
 Fungal infections of the nails are also known as onychomycosis, as tinea unguium, and as ringworm of the nails. The fungi in question are usually those that cause athlete’s foot — a common infection of the skin of the feet. In athlete’s foot the fungi live in the keratin that makes up the outer layer of the skin, but they can also invade the hard keratin of which nails are made. When this happens, the result is a fungal infection of a nail.
Fungal infections of the nails are also known as onychomycosis, as tinea unguium, and as ringworm of the nails. The fungi in question are usually those that cause athlete’s foot — a common infection of the skin of the feet. In athlete’s foot the fungi live in the keratin that makes up the outer layer of the skin, but they can also invade the hard keratin of which nails are made. When this happens, the result is a fungal infection of a nail.
What causes onychomycosis?
Fungi spreading from athlete’s foot (known as ‘dermatophyte fungi’) cause most fungal nail infections.
Far less often a nail infection is due to other types of fungi, usually yeasts (eg. Candida) and moulds (e.g. Scopulariopsis), which do not cause athlete’s foot. These like to attack nails that are already weak, perhaps after an old injury. Fungal infections of toenails are common, those of fingernails far less so. Both are seen most often in the elderly.
Are they hereditary?
No, but several family members may have them at the same time because they can catch them from each other.
What are the symptoms of fungal infections of the nails?
At the start, there are usually no symptoms. Later the nails may become so thick that they hurt when they press on the inside of a shoe. They are then hard to trim. The look of an infected nail, particularly a fingernail, can be embarrassing.
What do fungal infections of the nails look like?
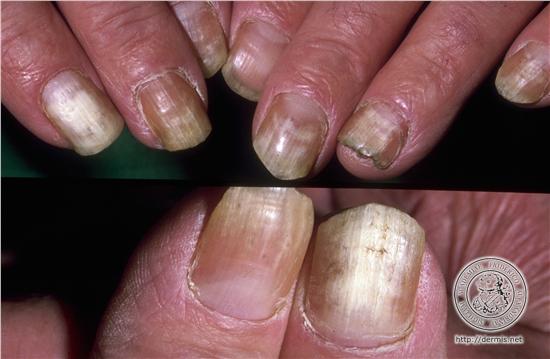
When fungi invade a nail, they usually start at its free edge, and then spread down the side of the nail towards its base. Eventually the whole nail may be involved. The infected areas turn white or yellowish, and become thickened and crumbly. Less common patterns of infection include white patches or streaks on the nail surface. The nails most commonly affected by fungal infections are those on the big and little toes. When several fingernails are infected, they are usually on the same hand.
How are fungal infections of the nail diagnosed?
Many nail problems can look like a fungal infection — for example the changes seen in psoriasis, or after a bacterial infection or an old injury — however, long courses of antifungal tablets will not help them. This is why the diagnosis of a fungal infection must always be confirmed before treatment starts. Your doctor will take a piece from a crumbly area of your nail and send it to the laboratory to check if a fungus can be seen under the microscope or grown in culture. The right treatment may depend on knowing which fungus is causing the trouble but it can take several weeks for the final culture results to come through.
Can fungal infections of the nails be cured?
Yes — usually they can.
How can fungal infections of the nails be treated?
Fungal infections of the nail do not clear up by themselves, but not all of them need treatment. Many people with infected toenails are not bothered by them at all. In that case they can be left alone. On the other hand, if infected nails are embarrassing or uncomfortable then they are usually worth treating.
The aim of the treatment is to get rid of the fungus: the nail will then usually return to normal. However, if the nail was abnormal before it picked up the fungal infection, it will be hard to clear and may just go back to its former state. Nail infections caused by moulds and yeasts can be very resistant to treatment.
Treatments applied to the nail
Treatments put on the nail do much less well than those taken by mouth. They work best if the infection is at an early stage, just on the free edge of one or two nails, or lying close to the surface of the nail. The preparations used most often are amorolfine nail lacquer and tioconazole nail solution. Alone, they may not be able to clear the deeper parts of an infected nail, though regular removal of abnormal nail material with clippers or filing can help with this. Used in combination with an antifungal remedy taken by mouth, they increase the chance of a cure. They may have to be used for a period of 4 to 12 months before a response is noted.
Treatment by mouth
Before starting you on tablets, your doctor will send a piece of your nail to the laboratory to check that the diagnosis of a fungal infection is correct.
Three medicines are available for use in fungal nail infections:
- Griseofulvin has been used for many years and is the only one of the three medicines licensed for use in children. It is only absorbed fully if taken with fatty foods, and long courses of treatment are usually needed (6 to 9 months for fingernails, and up to 18 months for toenails). Even so, only about three quarters of infected fingernails and one third of infected toenails will clear up. Relapses are common.
- Terbinafine and itraconazole have largely taken over from griseofulvin now. They work better and much more quickly. Cure rates are 80 to 90% for fingernails, and about 70% for toenails.
- Terbinafine works best against dermatophyte fungi (the ones that cause athlete’s foot). It is taken daily for 6 weeks for fingernail infections and for 12 weeks for toenail infections.
- Itraconazole acts against dermatophytes too, although usually it is not quite as effective as terbinafine; but it is also active against other fungi such as yeasts. It is often given in bursts — for one week in every month. Two of these weekly courses, taken 21 days apart, are usually enough for fingernail infections and three for toenail infections.
Remember that the new normal nail will grow slowly outward from its base, and it may be 6 months to a year after the treatment has finished before the nails look normal again. Fingernail infections clear up more quickly and completely than toenail ones.
Surgical removal of nails
Sometimes very thick nails that are not likely to respond to tablets alone may have to be removed under a local anaesthetic.
- Self care (What can I do?)
- Keep your nails short, dry, and clean. Stick to one nail clipper for the infected nails and another for the normal ones.
- Don’t just treat your nails; use an antifungal cream to treat the skin that has athlete’s foot as well.
- Keep your feet dry, wear cotton socks, changed daily, and use ‘breathable’ shoes.
- Your activities need not be limited during treatment but, to avoid a recurrence, don’t walk barefoot around public pools, showers, and locker rooms

